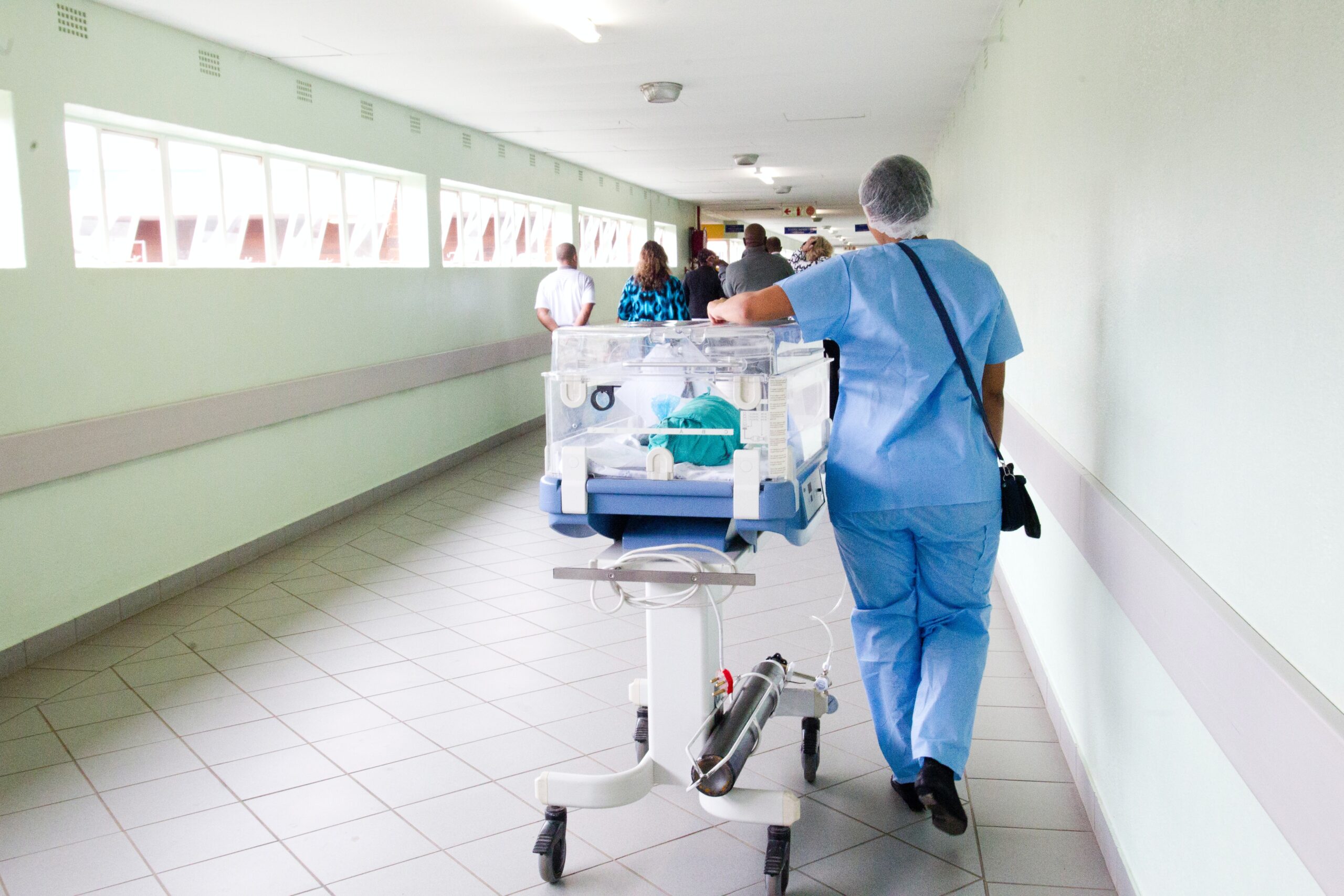
The pandemic has pushed medical professionals squarely into the spotlight around the world. As we continue to face one of the biggest global challenges to public health in generations, never more has the country been so grateful to our doctors and nurses on the frontline. Nurses have been labeled “heroes” by politicians, the mass media, and the general public to describe their commitment to providing front-line care to people with COVID-19, despite the risks of exposure and lack of clinical resources. But at what cost has the label ‘hero’ been applied?
In the article Angels and Heroes: The Unintended Consequence of the Hero Narrative, the authors conclude that “in summary, while the description of nurses as heroic may be noble, we emphasize that the unintended consequences may be more harmful than the intent. Nurses are skilled critical thinkers, strong leaders and managers, compassionate patient advocates, dexterous practitioners, and empathetic communicators, but they are not angels or heroes.”
These ‘unintended consequences’ are around the fact that heroes aren’t supposed to complain, or to speak out about unrelenting work patterns, burnout, or chronic stress. Elsevier Health, a provider of information solutions for science, health and technology professionals, conducted its first “Clinician of the Future” global report. It revealed current pain points, predictions for the future and how the industry can come together to address gaps—including that 31% of clinicians globally, and 47% of U.S. healthcare workers, plan to leave their current role within the next two to three years.
Clearly then, this language of heroism is causing problems and masking the true feelings of our nursing professionals. Instead it’s proving to be the kind of lip service that’s increasingly difficult for nurses to distance themselves from. What nurses need is adequate staffing, PPE, security and access to mental health resources. We shouldn’t expect heroism from nurses. Instead, we should expect professionalism in the context of a well-run health service.
Even before the pandemic, research showed that nurses face great mental health challenges. In a 2020 University of California at San Diego study, it was found that there was a higher rate of suicide among nurses than the general population. In a further Mayo Clinic study from October 2021, nurses, pre-pandemic, had more suicidal thoughts than other workers but were less likely to tell anyone.
At a time when nurses are most needed, more needs to be done by health systems and employers to recognize the challenges that nursing staff are facing and actively designing and deploying new strategies to stop nurses from leaving the profession in their droves.
A 2021 McKinsey study offered the following 4 strategies to stem the flow:
- Make workforce health and well-being part of the fabric. Nurses, similar to employees across all sectors, are looking for more support from the organizations that employ them. Recognition (appreciation and economic rewards commensurate with their value), communication, and breaks to recharge are paramount. Also important are increased availability and accessibility of resources (for example, mental health resources).
- Increase workforce flexibility. COVID-19 accelerated the introduction of scheduling and staffing approaches to create additional flexibility in workforce deployment.
- Reimagine delivery models. Organizations may consider how to leverage digital tools and adapt care models based on patient and employee preferences. For example, some employers may continue (or expand) clinician use of telemedicine platforms, allowing nurses to work remotely more often.
- Strengthen talent pipelines and build skills for the future. Demand for talent is increasing, and skill sets and capabilities required are shifting. Organizations will need to re-skill in some areas, as well as bolster their recruiting pipeline for clinical roles—in some cases leaning on new partners or professional development pathways.
The McKinsey study suggested that health systems, higher education institutions, the public sector and others have recognized there is a critical need and a time-sensitive opportunity to recommit to the support and development of the nursing workforce.
This is why at Seacole we do things differently. We offer a new approach to healthcare employment that supports flexible working and values mental wellbeing as highly as individual contribution. We believe that to ensure all nurses are set up for success, they need support from their employer and flexibility in their working model, not capes.
Start your journey to a better future today
Don’t hesitate to get in touch with us today to learn more about making a positive difference on your own terms.
Click here to get in touch.



